In 1983, Dr. J. Robin Warren and Dr. Barry Marshall reported finding a new kind of bacteria in the stomachs of people with gastritis. Warren and Marshall were soon led to the hypothesis that peptic ulcers are generally caused, not by excess acidity or stress, but by a bacterial infection. Initially, this hypothesis was viewed as preposterous, and it is still somewhat controversial. In 1994, however, a U. S. National Institutes of Health Consensus Development Panel concluded that infection appears to play an important contributory role in the pathogenesis of peptic ulcers, and recommended that antibiotics be used in their treatment. Peptic ulcers are common, affecting up to 10% of the population, and evidence has mounted that many ulcers can be cured by eradicating the bacteria responsible for them.
This paper is the first of two that discuss the development and reception of the bacterial theory of ulcers from a combination of historical, methodological, psychological, and social perspectives. It examines the nature of the discoveries made by Marshall and Warren, including the new bacteria now known as Helicobacter pylori, the hypothesis that peptic ulcers are often the result of bacterial infection, and the hypothesis that peptic ulcers can be cured by treatment with antibiotics. This paper also describes the kinds of conceptual change that attended the adoption of the new hypotheses. It then examines the reasons for the initial rejection of the bacterial theory of ulcers as well as the reasons for its increasing acceptance. It discusses how causal hypotheses can be established in medical research and analyzes the acceptance and rejection of the bacterial theory of ulcers in terms of explanatory coherence. The perspective in this paper is cognitive, considering the mental operations that produced the discovery and acceptance of the bacterial theory of ulcers.
The sequel (Thagard, forthcoming-b), looks at the same case from physical and social perspectives. The development of the bacterial theory of ulcers depended on the physical use of instruments such as microscopes and endoscopes, and on the devising of experiments to test the association of Helicobacter pylori and gastric problems. It also had important social dimensions, including: the collaborative work of Marshall, Warren, and their associates; the processes of communication by which the new concepts and hypotheses spread; and the processes of negotiation by which consensus began to form, for example on the NIH panel. This paper shows how social explanations of scientific development can complement psychological and methodological explanations. The two Ulcers and Bacteria papers together give a broad, integrated, naturalistic explanation of a recent episode in medical science, treating science as a complex system of interacting cognitive, physical, and social processes.
In the past decade, a dramatic shift has occurred in the understanding and treatment of peptic ulcers, which are now widely (although not universally) viewed as bacterial in origin and treatable by antibiotics. The shift originated with the work of two Australian physicians, Robin Warren and Barry Marshall. After sketching the history of the discoveries concerning gastric bacteria and peptic ulcers, I will describe four current models of scientific discovery and show how the models contribute to explanation of the three discoveries.
Spiral bacterial had been previously observed in the stomachs of various carnivores, including humans, but they were not viewed as medically significant. In 1981, Barry Marshall began a six-months gastroenterology assignment as part of his training program in internal medicine. The chief of gastroenterology suggested that Marshall help Warren investigate the bacteria he had observed. Warren and Marshall noticed similarities between the gastric spiral bacteria and bacteria of the genus Campylobacter. In April, 1982, the spiral organism was cultured for the first time, and it became apparent that this was a new species of bacteria, given the name Campylobacter pyloridis in 1983. (The pylorus is the opening from the stomach into the duodenum, which is the first part of the intestine.) In 1987, the name was corrected to Campylobacter pylori, but RNA analysis and other studies led to the determination that the bacteria did not belong in the genus Campylobacter, and the name was changed again to Helicobacter pylori (Goodwin et al., 1989). Several other species of the genus Helicobacter are now recognized in ferrets, cats, and dogs. Since 1983, more than 3,000 papers have been published on Helicobacter pylori.
Although the hypothesis that peptic ulcers are caused by bacteria was initially viewed as preposterous by many gastroenterologists, subsequent studies have largely supported the claim of Marshall and Warren, and the hypothesis is taken seriously even by those who still contend that the issue is unsettled. Sections 7-11 review the considerations that affected the initial rejection of the hypothesis that H. pylori causes ulcers and its subsequent widespread acceptance.
Schunn and Klahr (1995) have proposed a model of discovery that involves search in four spaces. They write (p. 106):
One fruitful characterization of scientific discovery is to view it in terms of search in two problem spaces: a space of hypotheses and a space of experiments (Klahr & Dunbar, 1988; Simon & Lea, 1974). ... In [Schunn and Klahr's] new framework, what has been previously conceived as the hypothesis space has now been divided into a data representation space and a hypothesis space. In the hypothesis space, hypotheses about causal relations in the data are drawn using the set of features in the current representation. Similarly, the old experiment space is now divided into an experimental paradigm space and an experiment space. In the experimental paradigm space, a class of experiments (i.e. a paradigm) is chosen which identifies the factors to vary, and the components which are held constant. In the experiment space, the parameter settings within the selected paradigm are chosen.New data representations can be produced by learning mechanisms such as concept formation and analogy (Holland, Holyoak, Nisbett, and Thagard, 1986).
Q1. Do species transmute?Q3 and Q2 are relevant to answering Q1, which also gave rise to the question of how species transmute, eventually answered by the theory of natural selection. Darwin's intellectual problem, however, was much too complex and ill-defined for us to specify a problem space in terms of states and operators, but we can nevertheless understand the development of his views in terms of a series of questions that he posed to himself. Various writers in philosophy, psychology, and artificial intelligence have emphasized the importance to inquiry of question generation and answering (Bromberger, 1992; Hintikka and Vandamme, 1985; Lauer, Peacock, and Graesser, 1992; Ram 1991).Q2. Are Galapagos specimens distinct species or distinct varieties?
Q3. Do the variations observable among the mockingbird specimens correspond to variations among acknowledged species?
Where do new scientific questions come from? Some are generated as subordinate questions designed to answer questions already posed. Truly original questions seem to arise from three major sources: surprise, practical need, and curiosity. Surprise occurs when something is found that is not coherent with previous expectations and beliefs, for example when Darwin found an unusual distribution of species in the Galapagos. Practical need generates scientific questions when the accomplishment of some technological task is seen to require additional knowledge about how the world works, as when the Manhattan project gave rise to questions in atomic physics crucial to building an atomic bomb. Curiosity generates questions when there is something that a scientist want to know out of general interest, not because of previous surprise or practical need. Here are schemas for four kinds of scientific question generation:
1. A scientist is surprised to learn information that does not cohere with existing knowledge.2. So the scientist asks for an explanation of the information.
1. A scientist has practical goals, for example medical or technological goals.2. The scientist is not aware of any means to accomplish these goals.
3. So the scientist asks how to accomplish the goals.
1. A scientist has considerable knowledge about a phenomenon P1.2. There is a phenomenon P2, similar to P1, but many kinds of information available about P1 are not available about P2.
3. So the scientist asks questions about P2 with potential answers similar to what is known about P1.
1. A scientist wants to answer a question Q1.Undoubtedly, this is not an exhaustive set of ways of generating scientific questions, but it will be useful for discussing discoveries about ulcers and bacteria.2. Answering question Q2 is relevant to answering Q1, because either:
(a) the answer to Q2 entails the answer to Q1;(b) the answer to Q2 might provide evidence relevant to an answer to Q1;
(c) the answer to Q2 is analogically relevant to an answer to Q1, because Q2 and Q1 are similar questions.
Advocates of the search model of discovery will likely argue that questioning can also be assimilated to search. Perhaps one could posit a "question space" to expand further Schunn and Klahr's (1995) 4-space model, arguing that researchers first search the question space and then move on to explore the other four spaces. But the putative question space, like their data representation space and experimental paradigm space, is so vast and ill-defined that I see little explanatory gain in describing it as being searched. The metaphor of discovery as search applies well to a hypothesis space where the representations are given and to an experimental space where the paradigms are given, but becomes unacceptably vague when stretched to cover uncharted territory.
Moreover, Schunn and Klahr's expanded model assumes, like the standard search model, that discoverers are working with a problem presented to them. It does not address the issue of problem generation, which is the same as the issue of how potentially fertile questions arise. So formation of interesting questions should not be assimilated to the search model. But questioning and search are related, in that the formulation of even vague questions can lead toward defining problems that can be solved by search. Once a question is formulated, subordinate questions relevant to answering can be suggested, and it may be possible to answer some of these by solving well-defined problems in a fashion appropriately characterized as search.
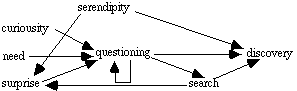
Similarly, serendipity may contribute to both questioning and search. Serendipity may provide a surprising or curiosity-inducing event that inspires questioning, as when Newton's perception of the fall of an apple moved him to wonder why objects fall toward the earth's center. Moreover, when a search is underway, serendipity may provide a representation or operator that was not part of the original problem space, as when Goodyear discovered vulcanization. Kantorovich (1993) views serendipity as a kind of blind variation, but is vague about what is varied. Ignoring blind variation, figure 1 shows the influence relations of serendipity, questioning, and search. Questioning arises from curiosity, need, and/or surprise, and can lead to discovery, search, or more questioning. Surprise can arise from serendipity or from the results of search. Discovery can be the result of various combinations of serendipity, questioning, and search. Let us now see how these models help to explain the three discoveries concerning bacteria and ulcers.

Figure 1. Interrelations of models of discovery
Serendipity also played a role in the efforts to culture the bacteria. During the 1970s, techniques for culturing Campylobacter had been developed, but thirty attempts in late 1981 to use these techniques to culture the gastric bacteria failed, partly, it was later discovered, because of faulty incubators. Agar plates on which the bacteria were supposed to grow had been discarded after forty-eight hours with no growth visible. Then in April, 1982, because of a four-day Easter weekend and other demands on the microbiology laboratory, the culture was left in the incubator for five days, long enough for bacterial colonies to become visible (Marshall, 1989, p. 14). This is an example of pseudoserendipity, since the investigators certainly had the goal of culturing the bacteria, but incubating for five days was not a method that they had been considering.
Surprise and curiosity led Warren to ask questions about the nature of these bacteria, and he requested a silver stain that made the number and shape of the microorganisms much more evident. Surprise was certainly a factor, since it was generally believed that the stomach is sterile. Curiosity was piqued by the fact that little was known about the stomach bacteria, in contrast to the vast amount of information available concerning other bacteria. Marshall joined in the questioning about the nature of the bacteria, stating in his part of the letter to Lancet: "The above description of S-shaped spiral bacteria in the gastric antrum, by my colleague Dr. J. R. Warren, raises the following questions: why have they not been seen before; are they pathogens or merely commensals in a damaged mucosa; and are they campylobacters?" (Warren and Marshall, 1983, p. 1273). Marshall engaged in a systematic literature search to try to find out whether they were members of a species already known. Thus the question "What are these bacteria?" gave rise to a fairly well-defined search to answer the question "Are these bacteria of any known species?" The answer to that question turned out to be negative, so initially a new species and eventually a new genus, Helicobacter, were generated. In the terms of Schunn and Klahr, this would be described as the result of a search through a space of representations, but that space is so ill-defined that the relevance of the search metaphor is dubious. Marshall (1989, p. 16), reported:
For me, identification of the bacterium posed a problem. None of the textbooks gave details concerning where to start when totally new bacteria are discovered. Most books merely told how to test if a bacterium was the same as, or different from, the known species. In a clinical laboratory this meant checking a new isolate against a panel of known pathogens and then discarding it if no match was made.The question of the nature of bacteria inspired a search for identification with known bacteria, but the failure of this search required the postulation of a new species.
In sum, the discovery of Helicobacter pylori is best described as the result of serendipity and surprise which produced questioning that led to search that produced more questioning that generated the recognition of a new species of bacteria.
The first step in the generation of this hypothesis was Warren's noticing of an association between the gastric spiral bacteria and gastritis. This association was obvious to him from his first observations of the bacteria, since in the biopsies he was examining it was clear that stomach cells close to the bacteria were damaged, whereas cells remote from bacteria were not. From Warren's perspective, observation immediately suggested a causal connection between the bacteria and stomach inflammation. But his attempts to interest gastroenterologists in the bacteria were unsuccessful until Marshall was assigned to do a research project with him.
As a practicing physician, Marshall naturally raised the question whether the newly discovered bacteria were pathogens. This question is inspired not merely by curiosity, but also by the professional need to treat illnesses. Marshall was aware that many stomach problems such as gastritis and ulcers could be reduced but not generally cured by antacids. The question "Are the bacteria pathogenic?" could be made more specific: "What gastric diseases might the bacteria produce?" Since there are only a relatively small number of such diseases, it was possible to search for disease correlates of the bacteria. The search took two forms, literary and experimental. During his extensive reading in the summer of 1982, Marshall encountered the repeated observation that chronic gastritis was associated with peptic ulcer (Marshall, 1989, p. 15). He already knew from Warren's work that gastritis and bacteria were associated. So it was natural to consider that the bacteria might be associated with peptic ulcer. Marshall designed a study aiming to "(1) decide if the bacteria were associated with gastritis, (2) find the source of infection, (3) culture the bacteria, and (4) determine which diseases, if any, were associated with infection" (Marshall, 1989, p. 13). The study conducted in 1982 looked for associations between stomach appearance as judged by endoscopy and occurrence of bacteria as indicated by biopsy. Bacteria were found in 77% of patients with gastric ulcers, and 100% of patients with duodenal ulcer, in contrast to 50% of patients with normal stomachs (Marshall and Warren, 1984, p. 1312).
Marshall's formation of the hypothesis that spiral bacteria cause ulcers thus depended on the following chain of associations:
1. Bacteria are associated with gastritis (Warren).Marshall and Warren (1984, p. 1314) concluded their paper by saying: "Although cause-and-effect cannot be proved in a study of this kind, we believe that pyloric campylobacter is aetiologically related to chronic gastritis, and, probably, to peptic ulceration also." The inference from step 4 to 5 seems to derive from a simple heuristic: If A and B are associated with each other, then they may be causally related. Once the search for associates of the bacteria turned up ulcers, the leap to considering a possible causal relation was automatic. Could it be, on the other hand, that ulcers cause bacteria by virtue of a stomach ulcer providing a fertile environment for bacteria to grow? Given the occurrence of bacteria in patients without ulcers, and the fact that the bacteria were not found to be prominent on gastric ulcer borders, it was more plausible that bacteria cause ulcers than vice versa.2. Gastritis is associated with ulcers (reading).
3. So maybe bacteria are associated with ulcers.
4. Bacteria are associated with ulcers (experimental study).
5. So maybe bacteria cause ulcers.
Thus the process of discovery of the hypothesis that ulcers are caused by bacteria included questioning leading to search and application of a heuristic to infer causality from association. Since the pioneering work of Marshall and Warren, Helicobacter pylori has also been implicated as a possible cause of stomach cancer and heart disease. Establishing that a correlated factor is indeed a cause is an extremely complex process that is discussed in sections 8 and 9.
1. Ulcers are associated with and may be caused by bacteria.The question whether ulcers can be cured by antibiotics converted immediately into a search for what antibiotics are most effective. Given the large amount of knowledge about treatment of bacterial infections available by the 1980s, this problem was relatively well-defined and the search was quite manageable. Marshall (1994) describes various regimens that are effective for eradicating H. pylori and curing many cases of peptic ulcers.2. Similarly infectious diseases (e.g. tuberculosis) caused by bacteria can be cured by antibiotics.
3. So perhaps ulcers can be cured by antibiotics too.
Thus the three discoveries about ulcers and bacteria varied in the extent of the roles played by serendipity, questioning, and search. Serendipity played a large role in the discovery of the spiral bacteria, while questioning seems most important to the formation of the hypothesis that bacteria cause ulcers, and search sufficed to find successful antibiotic treatments for ulcers.
The two kinds of conceptual change most relevant to the ulcer/bacteria case are concept formation and reclassification. Concept formation involves the generation of new concepts such as Helicobacter pylori, while reclassification involves revision in the kind relations that organize concepts in mental systems. In cognitive psychology, psycholinguistics, and artificial intelligence, it is widely agreed that conceptual systems are structured in large part by kind relations: a robin is a kind of bird which is a kind of animal which is a kind of thing. Reclassification involves moving a concept from one branch in the tree of concepts to another branch.
Undoubtedly, the most important concept formed during the development of knowledge about ulcers and bacteria was the concept of Helicobacter pylori, and we have already seen that the formation of this concept was historically complex. Warren and Marshall did not simply observe a host of bacteria and dub them with the name Helicobacter pylori. Initially, they used the informal term "gastric spiral bacteria", thus forming a concept by combining existing well-established concepts. The process of conceptual combination is sometimes intersective, producing a new concept that involves the intersection of existing concepts: spiral bacteria are just bacteria that are spiral (see Thagard, 1988, for a discussion of this kind of conceptual combination as a mechanism of discovery). But other conceptual combinations produce puzzlement that leads to emergent properties. Kunda, Miller, and Claire (1990) presented subjects with surprising examples like "blind lawyer" and found that combination often involved generation of aspects not part of the original concepts; for example, a blind lawyer may be hypothesized to be courageous in order to explain how someone who is blind could become a lawyer. The conceptual combination "gastric bacteria" is of just this sort, since before Warren's work it was widely believed that the stomach was too acidic for bacterial colonization. Hence the new combination provoked the question: "How can bacteria live in the stomach?" The interesting answer is that members of H. pylori bury themselves beneath the mucosal layer and produce ammonia which neutralizes the gastric acid. So the anomalous combination "gastric bacteria" led to an emergent property, ammonia- producing.
Initially, Warren and Marshall thought that the gastric spiral bacteria might be members of a known species of the genus Campylobacter. Had this been so, no concept formation would have been necessary, since the newly discovered objects would have been assimilated to an existing concept. Concept formation often involves differentiation, in which an object or substance is distinguished from ones already conceptualized. Once it became clear that the gastric bacteria did not fall under any known species, it was appropriate to differentiate them under the heading of Campylobacter pylori.
From the start, however, it was clear that the flagellar morphology of the gastric bacteria, which have several sheathed flagella at one end, differed from members of the genus Campylobacter, which have a single unsheathed flagellum at one or both ends (Marshall and Warren, 1984). RNA analysis and other studies eventually showed that the new bacteria are sufficiently distinct from campylobacters to warrant assignation to a new genus, Helicobacter. Conceptual change thus involved both formation of new concepts for the genus Helicobacter and the species Helicobacter pylori, but also reclassification of the new species as Helicobacter rather than as Campylobacter.
Reclassification of diseases is required for acceptance of the hypothesis that ulcers are caused by bacteria. Marshall remarked that "the C. pylori story will mature, in my opinion, when medical texts have a chapter on peptic ulcer disease within the infectious disease section" (Marshall, 1989, p. 21). Current medical textbooks organize their discussions of diseases in two parallel ways, in terms of organ system affected (e.g. cardiovascular diseases, respiratory diseases) and pathogenesis (e.g. infectious diseases, oncology). The hypothesis that ulcers are caused by bacteria requires reclassification of the disease as an infectious disease, where previously it was viewed as caused by acid imbalance and was sometimes even classified as psychosomatic. Reclassification of ulcers as an infectious disease goes hand in hand with decision to treat them with antibiotics.
Moreover, ulcers can be further classified in terms of how various types are caused: "We now recognize at least three types of duodenal ulcer disease: H. pylori-related, NSAID-associated, and hypersecretory" (Graham, 1991, p. 108). Thus ulcers can now be viewed as consisting of several kinds, including the kind associated with bacterial infection. Accepting a bacterial cause for most ulcers made possible reclassification of ulcers as an infectious disease, but also required the subdividing of ulcers into infectious and non-infectious subkinds. The concept Helicobacter pylori has also been subject to subcategorization, since two different strains have been suggested, one of them more likely to produce a peptic ulcer than the other (Monmaney, 1993).
The discovery of also led to a change in the concept of gastritis. Marshall (1989, p. 16) says of the 1982 study: "It then became clear that only people with gastritis had the gastric spiral bacteria. We therefore had an association between the bacterium and a condition that was at the time not even recognized as a disease." Previously, gastritis was considered to be so common and to have so many possible causes that it was not considered to be a disease. But once a specific bacterial cause was identified, it became possible to reclassify histological gastritis as a bacterial disease. Warren and Marshall's advocacy of such a reclassification still encounters resistance from some gastroenterologists.
Although appreciation of the bacterial theory of ulcers requires the construction and reorganization of concepts, it would be a gross exaggeration to suggest that the new theory of ulcers was incommensurable with the old. Critics of Warren and Marshall did not have trouble understanding the claim about ulcer causation; the critics just thought the claim was wrong, or at least undemonstrated. Once evidence accumulated in support of the claim, its acceptance became widespread (see section 10).
Of course, the process of discovery is much more complex than either figure 1 or figure 2 presents. As we saw in section 4, the growth of knowledge about ulcers and bacteria was not just a matter of generation of hypotheses, but also required considerable conceptual change, including both formation of new concepts and reclassification of existing ones. Conceptual systems interact with discovery algorithms in ways suggested by figure 3, which also points to the physical role of instruments and experiments and to the social role of collaboration discussed in the sequel (Thagard, forthcoming-b). Moreover, the generation of hypotheses is not equivalent to their acceptance, since alternative explanations must be considered, as I will now discuss.Figure 2. Discovery as generation of hypotheses from data.
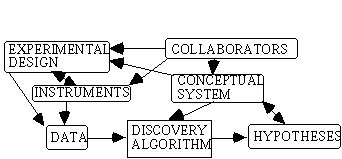
Figure 3. Discovery as a complex cognitive, physical, and social process.
Hypothesis 1: Gastric spiral bacteria (Helicobacter pylori) inhabit the human stomach.I now want to discuss how these hypotheses have been evaluated by medical researchers and why they have become increasingly accepted.Hypothesis 2: These bacteria can cause peptic ulcers.
Hypothesis 3: Peptic ulcers can be cured with antibiotics.
The two central questions are how the cause of a disease can be ascertained by medical research, and how researchers can change their minds about what causes a disease. Marshall and Warren's (1984) suggestion that ulcers may be caused by bacteria was initially viewed by some researchers as absurd and outrageous. Martin Blaser of the Division of Infectious Diseases at the Vanderbilt University School of Medicine thought a 1983 talk by Marshall was "the most preposterous thing I'd ever heard; I thought, This guy is a madman." (Monmaney, 1993, p. 65). Blaser (1989, Cover and Blaser, 1992) has since become one of the leading researchers on Helicobacter pylori. Dr. David Forman of the Imperial Cancer Research Fund thought that Marshall's claim that bacteria are responsible for various stomach diseases including cancer was a "totally crazy hypothesis" (Suzuki, 1995, p. 9). But he thought it worth demolishing, and since has concluded that Helicobacter pylori infection is a major factor in gastric cancer as well as ulcers (Forman et al., 1991; EUROGAST Study Group, 1993). Other gastroenterologists were skeptical of Marshall and Warren's claims, but sufficiently intrigued to launch their own research programs.
I will try to explain why the hypotheses about ulcers and bacteria seemed crazy to many in 1983, but why Marshall and Warren nevertheless accepted them. Section 7 describes Marshall's early attempts to convince others of the causal role of H. pylori using Koch's postulates, a time-honored method of establishing particular bacteria as causes of a particular disease. Koch's postulates require that the bacteria be transmitted to an uninfected animal and produce disease in it; the postulates have been fulfilled for gastritis, but not for ulcers. I will identify the causal reasoning that underlies application of Koch's postulates, and argue that they are a sufficient but far from necessary means for establishing causality (section 8). In addition to a large amount of correlational evidence linking the ulcers and bacteria, numerous experiments have shown that peptic ulcers can be cured by antibiotics. Section 9 describes how acceptance of hypothesis three, that antibiotics cure peptic ulcers, provides major support for hypothesis 2, that ulcers are caused by bacteria. Accepting that bacteria cause ulcers is a major part of the belief change experienced by many medical researchers in the decade between 1985 and 1995, but other interconnected beliefs are also involved. Section 10 shows how the shift to the bacterial theory of ulcers can be understood in terms of an account of explanatory coherence that has been widely applied to conceptual revolutions in the natural sciences.
Hypothesis 1, that members of a previously unidentified species of bacteria inhabit the human stomach, was initially greeted with incredulity because of prevailing beliefs about the stomach. According to Blaser (1989, p. 1), "most physicians believed that the normal human stomach, because of its high acid concentration, was sterile except for transient bacterial flora." Hypothesis 1, however, was quickly established as numerous researchers who had specialized in research on Campylobacter infections in humans turned their attention to what was taken to be a new species of that genus. The new bacteria could be microscopically observed using the staining techniques introduced by Warren, and they could be grown in the laboratory using the culturing techniques developed by Marshall. The apparent conflict between the acidic nature of the stomach and the existence there of bacteria has been resolved by discoveries about the nature of H. pylori. These bacteria are able to burrow beneath the mucous layer in the stomach, and they produce an enzyme, urease, that uses urea present in the gastric juice to generate ammonia, an alkaline that neutralizes acid (Marshall, et al., 1990). Bacteriologists were therefore quick to accept the hypothesis that a newly recognized kind of bacteria inhabit the human stomach.
Many gastroenterologists, however, found it much more difficult to consider a challenge to accepted views about the causes of peptic ulcers. By the early 1980s, it was widely believed that excess stomach acid is the main cause of peptic ulcers. People with increased amounts of acid were found to me more likely to get the disease, and cimetidine (brand name Tagamet) and ranitidine (brand name Zantac) were found to be effective antacid means of healing ulcers. Physicians thus had both an explanation in terms of excess acidity of why some people get ulcers, and an effective means of treating those people with Tagamet and Zantac, which remain among the most widely prescribed drugs. Hence hypothesis 2 that ulcers are caused by bacteria clashed with the hypothesis that acidity is the main culprit in peptic ulceration, and hypothesis 3 clashed with the effective standard treatment. It is not surprising, therefore, that many gastroenterologists rejected the new hypotheses as incoherent with what was already known (see section 4). Hence Marshall, a young, unknown Australian who put forward his new hypotheses with confidence amounting to brashness, was viewed as crazy.
In retrospect, however, there were problems with the accepted view of ulcers. It was not known why some people have excess acidity, although conjectures were made about genetic factors and psychological factors such as stress. The popular view of ulcers as a psychosomatic, stress-induced disease had given way to the emphasis on excess acidity, but stress remained one possible indirect explanation of ulcers, since it was known that stomach acid secretion increases in animals under stress. Even more important, although antacid drugs were usually effective in controlling the symptoms of ulcers, it was well known that recurrence of ulcers was common: the drugs clearly did not produce a cure. Hence when Marshall began to develop alternative hypotheses about the causes and treatment of ulcers, some researchers took them seriously enough to test them. Marshall, Warren, and their collaborators undertook to accumulate evidence concerning the cause and treatment of ulcers.
1) The parasitic organism must be shown to be constantly present in characteristic form and arrangement in the diseased tissue.Variants of these postulates have been used by generations of microbiologists as a description of what it takes to show that a microorganism is the cause of a disease.2) The organism which, from its behavior appears to be responsible for the disease, must be isolated and grown in pure culture.
3) The pure culture must be shown to induce the disease experimentally.
By 1984, Marshall and Warren had satisfied postulates 1 and 2, having shown a strong correlation between H. pylori infection and both gastritis and peptic ulcer. But initial attempts to satisfy postulate 3 using pigs were unsuccessful, so Barry Marshall undertook to experiment on himself. After endoscopy to show that he was free of gastric disease, he swallowed a flourishing three-day culture of the bacteria. After a week, he vomited and developed putrid breath, and biopsy showed that he had gastritis and his stomach contained the spiral bacteria (Marshall et al., 1985). Hence Koch's postulates had been fulfilled to establish that H. pylori infection causes gastritis. Since then, Koch's third postulate has also been satisfied by transmission of gastritis to bacteria-free piglets.
As of 1995, Koch's third postulate had not, however, been fulfilled for peptic ulcers. Marshall's self-induced case of gastritis cleared up on its own, so he did not have the continuing infection that might have contributed to an ulcer. In fact, most people who have H. pylori infections do not get ulcers. John Graham (1995) used the lack of fulfillment of Koch's postulates to cast doubt on the hypothesis that ulcers are caused by bacteria and contended that H. pylori is nothing more than an opportunist that accompanies ulcers. He maintained (p. 1096) that "as long as Koch's postulates remain unfulfilled for H. pylori as a cause of peptic ulcers or gastric malignancy, it is quite wrong for authoritative medical bodies to attempt to produce consensus documents that suggest that the eradication of H. pylori is an essential component of preventive or healing therapy." He thus challenged the 1994 NIH report that recommended such therapy (National Institutes of Health Consensus Development Panel, 1994).
If Koch's postulates were indeed a necessary condition of showing that a microorganism causes a disease, then we would have to delay accepting the hypothesis that bacteria cause ulcers. But the history of medical microbiology shows that, although Koch's postulates help to provide a convincing demonstration of a causal relation, they are not the only means of establishing causality. Koch himself encountered difficulty in fulfilling the third postulate (transmission of disease) for cholera, which he was convinced was caused by a bacterium even thought it did not produce the disease in any other animal. Even today, there are diseases such as typhoid fever and leprosy that cannot be reproduced in experimental animals with features resembling the human illness; nevertheless, their microbial causes have long been recognized (Evans, 1993, p. 31). Koch's second postulate (growth in culture) is also not always satisfiable: the microorganisms responsible for leprosy, syphilis, and malaria still elude growth in pure culture. Moreover, the second postulate does not apply at all to viruses, which cannot be grown in pure culture.
Why is fulfillment of Koch's postulates such an impressive demonstration of causality? Fulfilling the first postulate merely shows correlation between an organism and a disease, and the correlation might be accidental or the result of another causal factor. Fulfilling the second postulate shows that the organism is a clearly identifiable agent that might be responsible for disease. Fulfilling the third postulate is significant because it involves an experimental manipulation: doing something with the potential causal agent, the microorganism, has a dramatic effect on the disease, introducing it to a new animal. Koch's third postulate is important, not because it has some special probative status, but because it is a vivid kind of manipulation.
Other kinds of manipulation are possible in medical microbiology. Pasteur demonstrated that the organisms he had isolated from diseases such as rabies could be used in attenuated form to prevent the diseases. Hence we should count prevention of a disease by means of attenuated organisms as a manipulation relevant to establishing causality, in addition to transmission of a disease. A third significant manipulation is cure of the disease by eradication of the organism. This kind of intervention was not available in Koch's day, since antibiotics were only developed in the 1930s and 1940s, but we shall see in the next section that it has played a major role in convincing many medical researchers that bacteria cause ulcers.
Since Koch, new technology has made available other kinds of information concerning diseases, such as determining whether antibodies to an agent are produced in people who acquire the disease. According to Evans (1993), Koch's postulates have not been fulfilled for relating Epstein-Barr virus to infectious mononucleosis, since the virus cannot be grown in the laboratory and a susceptible experimental animal has not been found. Evidence has accumulated, however, that antibody to the virus is regularly absent prior to illness and regularly appears during clinical infectious mononucleosis. Table 1 shows the ten criteria for causation that Evans (1993) offers for establishing a cause for a disease.
Evan's criterion 1, prevalence, is satisfied for peptic ulcers and H. pylori as shown by the original study of Marshall and Warren (1984) and much subsequent research. I am not aware of studies showing that criteria 2-6 have been satisfied. Criterion 7, a weaker form of Koch's third postulate, has not been satisfied for peptic ulcers, which have not been experimentally reproduced. But criteria 2-7 are meant to provide only various sources of evidence concerning causal relations, not necessary conditions for demonstrating causality. Evan's criterion 8, that elimination of the putative cause should decrease the incidence of the disease, has been strikingly employed in the bacteria and ulcers case as section 9 discusses. Criterion 9, prevention of the disease, has not yet been satisfied, although work on a vaccine for H. pylori is underway. Criterion 10 is a very general condition that a causal hypothesis fit with other biological knowledge; its relevance to the ulcers and bacteria case is discussed in section 10.
| 1. Prevalence of the disease should be significantly higher in those exposed to the putative cause than in matched controls not so exposed. |
| 2. Exposure to the putative cause should be present more commonly in those with the disease than in controls without the disease when all risk factors are held constant. |
| 3. Incidence of the disease should be significantly higher in those exposed to the putative cause than in those not so exposed as shown in prospective studies. |
| 4. Temporally, the disease should follow exposure to the putative agent with a distribution of incubation periods on a bell-shaped curve. |
| 5. A spectrum of host responses should follow exposure to the putative agent along a logical biologic gradient from mild to severe. |
| 6. A measurable host response following exposure to the putative cause should regularly appear in those lacking this before exposure (i.e., anti-body, cancer cells) or should increase in magnitude if present before exposure; this pattern should not occur in persons not so exposed. |
| 7. Experimental reproduction of the disease should occur in higher incidence in animals or man appropriately exposed to the putative cause than in those not so exposed; this exposure may be deliberate in volunteers, experimentally induced in the laboratory, or demonstrated in a controlled regulation of natural exposure. |
| 8. Elimination or modification of the putative cause or of the vector carrying it should decrease the incidence of the disease (control of polluted water or smoke or removal of the specific agent). |
| 9. Prevention or modification of the host's response on exposure to the putative cause should decrease or eliminate the disease (immunization, drug to lower cholesterol, specific lymphocyte transfer factor in cancer). |
| 10. The whole thing should make biologic and epidemiologic sense. |
Marshall and Warren (1984, p. 1314) remarked of their study that found a strong correlation between bacterial infection and ulcers: "Although cause-and-effect cannot be proved in a study of this kind, we believe that pyloric campylobacter [H. pylori] is aetiologically related to chronic antral gastritis and, probably, to peptic ulceration also." In 1985 and 1986, they collaborated with the microbiologist C. Stewart Goodwin and other researchers on a prospective double-blind trial of duodenal ulcer relapse after eradication of the bacteria. One hundred patients with both duodenal ulcer and H. pylori infection were randomly assigned to eight weeks of treatment with either cimetidine or bismuth, and with either the antibiotic tinidazole or a placebo, producing four treatment groups. (The rationale of details of the experiment and the nature of the collaboration it required are discussed in Thagard, forthcoming-b.) The major result was that ulcer healing occurred in 92% of patients in whom H. pylori was not detected at 10 weeks, whereas only 61% of patients with persistent H. pylori healed. After 12 months, relapse occurred in 84% of patients in which H. pylori had not been eradicated, but in only 21% of the patients without continuing H. pylori infection. Marshall et al. (1988) concluded that the results imply that H. pylori is the most important etiological factor so far described for duodenal ulcer. A seven-year follow up examination found that an active ulcer remained in 20% of H. pylori-positive patients, but in only 3% of H. pylori-negative patients (Forbes et al, 1994). Similar results have been reported by Coghlan et al. (1987) and by Rauws and Tytgat (1990).
Between 1988 and 1990, David Graham and his colleagues in Houston compared patients (with ulcers and H. pylori infection) receiving (1) ranitidine versus (2) ranitidine plus triple therapy, consisting of bismuth and two antibiotics, tetracycline and metronidazole. After two years, they found that continuing infection with H. pylori was a strong predictor of ulcer recurrence (Graham et al., 1992). All 47 patients whose ulcers healed while receiving ranitidine still had H. pylori infection at the end of therapy, and 95% of them developed ulcer recurrence. In contrast, none of the patients in whom H. pylori was eradicated became reinfected. The effect was almost as strong for gastric ulcer as for peptic ulcer. Graham confidently editorialized that H. pylori infection is the most common known cause of peptic ulcer and accounts for the majority of cases, and that H. pylori ulcer disease can be cured (Graham, 1993; Graham and Go, 1993).
Critics of the bacterial theory of ulcers argued that the provision of bismuth might be the cause of ulcer healing in such experiments rather than eradication of the bacteria (Peterson, 1991). Bismuth produces dark stools, so the patients were not really blind to which treatment they had received, and bismuth might have an effect on the mucous layer that is more important than its known antibacterial properties. But Austrian researchers found that giving amoxicillin and metronidazole without bismuth was also a very successful treatment for duodenal ulcer, which recurred in 85% of patients given only ranitidine, but in only 2% of patients given ranitidine and antibiotics (Hentschel et al., 1993). Dutch researchers did a study to determine how important acid inhibition was to the eradication of ulcers, and found that triple therapy with bismuth, tetracycline, and metronadizole alone provided a 83% cure rate, compared to 98% with the addition of the acid inhibitor omeprazole (de Boer et al., 1995). Thus the acid inhibitor clearly helps, but the antibiotic treatment alone is highly effective for curing ulcers (Hosking et al., 1994). Antibacterial drugs, not just bismuth and antacids, play a key role in curing ulcers.
The U.S. National Institutes of Health regularly convenes consensus development conferences to make recommendations concerning medical treatments. The conference that met in February of 1994 produced a consensus document that ulcer patients with H. pylori infection be treated with antibiotics. The document stated that "the strongest evidence for the pathogenic role of H. pylori in peptic ulcer disease is the marked decease in recurrence rate of ulcers following the eradication of infection. The prevention of recurrence following H. pylori eradication is less well documented for gastric ulcer than for duodenal ulcer, but the available data suggest similar efficacy" (National Institutes of Health Consensus Development Panel, 1994, p. 66). Despite some remaining skepticism, medical discussion is clearly shifting away from whether bacteria cause ulcers to how best to treat the bacteria that cause ulcers. Correlational studies have also suggested that H. pylori is a causal agent in the development of gastric cancer and coronary heart disease, although these hypotheses have not yet been supported by studies that produce cures.
Thus the causal role of H. pylori in peptic ulcers seems to have been established without satisfying Koch's third postulate. Manipulation involving the transmission of disease is only one kind of evidence for causality. Acceptance of the hypothesis that peptic ulcers are caused by H. pylori depends on assessing various kinds of evidence in the context of alternative hypotheses. The next section lays out the evidential structure now supporting the bacterial theory of ulcers.
An important philosophical question remains: What does it mean to say that bacteria cause ulcers? A Humean regularity theory of causality would interpret it as saying that the bacteria and ulcers are universally associated, but this is clearly not the case: many people with H. pylori infection do not get peptic ulcers, and some cases of peptic ulcers occur because of use of non-steroidal anti-inflammatory drugs such as aspirin and ibuprofen. Approximately 30% of gastric ulcers are thought to be related to NSAIDs. A probabilistic theory of causality would note that the probability of ulcers given H. pylori infection is much higher than the probability of ulcers otherwise. This is true, but irrelevant if the increased probability is accidental or the result of a common cause that encourages both ulcers and bacteria. Medical researchers want to know why the probability of getting ulcers is so much greater in people with H. pylori infection. To answer this question, they are now investigating causal mechanisms such as one proposed by Graham (1990) in figure 4. It now appears that H. pylori infection increases acid secretion, and figure 1 suggests a series of processes by which infection can lead to gastrin release, acid secretion, and eventually to ulcer. Research is underway to fill in the gaps about these processes (Olbe et al., 1996). The statement that bacteria cause ulcers is thus not a comment about regularities or probabilities, but is rather an assertion that there is a continuous process connecting infection and the development of ulcers (cf. Salmon, 1984; Schaffner, 1993).
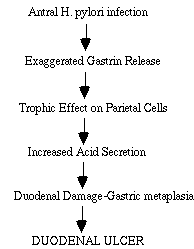
Figure 4. The role of H. pylori infection in the pathogenesis of exaggerated gastrin release and its theoretical role in patients with duodenal ulcer. Adapted from Graham (1990), p. 307. Graham elsewhere indicates that the causality is still more complicated, involving environmental factors, genetic predispositions, and possible interaction of acid secretion and bacterial infection.
The most powerful alternative to a coherentist explanation is Bayesian: one could say that the hypothesis that bacteria cause ulcers was improbable given the evidence in 1983, but probable given the evidence in 1995. To work this out in sufficient detail to apply Bayes theorem, one would need to specify numerous probabilities such as the prior probability of the hypothesis that bacteria cause ulcers, the probability of each piece of evidence given that hypothesis, and the probability of each piece of evidence. I know of no way of arriving at non-arbitrary values for such probabilities, nor of any plausible interpretation of the meaning of such probabilities, which are obviously very different from frequencies of occurrences of events in populations. Moreover, the aim in this series of papers is to provide a naturalistic explanation of scientific developments, so the explanation of belief change must be psychologically plausible. There is abundant evidence that human psychology often deviates from the canons of probabilistic reasoning (Kahneman, Slovic, and Tversky, 1982). Hence I shall pursue a much simpler and more psychologically plausible line of explanation based on coherence (2).
The kind of coherence most relevant to the evaluation of the hypothesis that ulcers are caused by bacteria is explanatory coherence. Thagard (1989, 1992) provides a set of principles for establishing coherence relations among hypotheses and evidence. For the ulcers/bacteria case, the most relevant principle is that when a hypothesis explains evidence or another hypothesis, the two proposition cohere with each other, so that there is a positive constraint between them, encouraging that either they both be accepted or both rejected. On the other hand, if two hypotheses contradict each other, or if they offer competing explanations of some piece of evidence, then they are incoherent with each other: this should lead to one of them being accepted and one rejected. Pieces of evidence are given priority, not in the sense that they must be accepted, but in the sense that there is a constraint that will encourage their acceptance. This constraint can be modelled by supposing that there is a special element EVIDENCE that is accepted and which coheres with all the pieces of evidence.
Let us now see why the hypothesis that ulcers cause bacteria was not coherent with most researchers beliefs in 1984 but was coherent for many researchers in 1995. Figure 5 provides a rough sketch of the positive and negative constraints on the various beliefs of a typical gastroenterologist in 1983. It shows that the hypothesis that ulcers are caused by gastric spiral bacteria was problematic for at least two reasons. First, it competed with the well-established hypothesis that peptic ulcers are caused by excess acidity. The most impressive evidence for this hypothesis was the healing of ulcers using drugs like Tagamet. Second, the hypothesis that gastric bacteria exist was incompatible with the accepted assumption that the stomach was too acidic for permanent bacterial growth. Since only a few researchers had observed the bacteria, and since there was only a small amount of evidence connecting ulcers and bacteria, it is not surprising that Marshall's hypothesis was greeted with incredulity. The bacteria that Warren observed could be explained as the result of contamination. Maximizing coherence, that is accepting and rejecting propositions in a way that maximizes the satisfaction of constraints, required rejecting the hypothesis that ulcers are caused by bacteria.
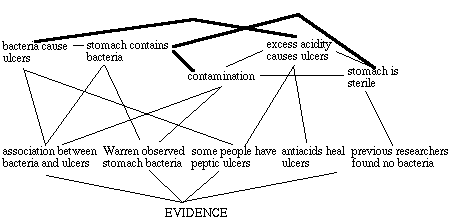
Figure 5. Coherence relations in assessing the acceptability of the hypothesis that bacteria cause ulcers in 1983. Thin lines indicated positive constraints based on hypotheses explaining evidence, and thick lines indicate negative constraints based on contradiction or competition.
Although figure 5 reflects the belief systems of many gastroenterologists at the time, the belief systems of Warren and Marshall were quite different. Warren's systematic observations made it clear to them that the stomach does contain gastric spiral bacteria and hence is not sterile; they knew that contamination was not a plausible explanation of Warren's results. Marshall was relatively new to gastroenterology but had a background in infectious diseases, so a bacteriological explanation of ulcers was less alien to him than to most gastroenterologists. But in 1983 their beliefs were at odds with accepted wisdom, and controlled studies to demonstrate a causal link between bacteria and ulcers had not been done.
By 1995, the picture had changed considerably. By then, countless researchers had studied Helicobacter pylori, so the view of the stomach as bacteria-free had dropped out altogether. Moreover, more than half a dozen studies from different researchers using different techniques had shown that ulcers can be cured using antibiotics that eradicate the bacteria. In addition, some researchers had conjectured that H. pylori increases acidity and that eradication of H. pylori decreases acidity. Figure 6 shows part of the coherence network involving hypotheses at that time. Maximizing coherence therefore requires accepting the hypothesis that ulcers are caused by bacteria. More constraints are satisfied if the hypothesis that bacteria cause ulcers is included in the set of accepted elements than if it is included in the set of rejected elements.
If explanatory coherence now requires accepting the bacterial theory of ulcers, why are some medical researchers still skeptical and why are many physicians still not treating ulcers with antibiotics? One reason is that communication is slow: the relevant research has only appeared in medical journals over the past few years, and practitioners have much to do besides reading medical journals. Another is that explanatory coherence is not the only kind involved in medical decisions, which are practical as well as theoretical. Treatment of peptic ulcers with Tagamet and Zantac is a tried-and-true way of making most ulcer patients feel better. Triple therapy with antibiotics and bismuth requires up to 15 pills a day and can produce nausea and diarrhea. Conservatism in adopting new treatments is not necessarily a bad trait in a medical practitioner.
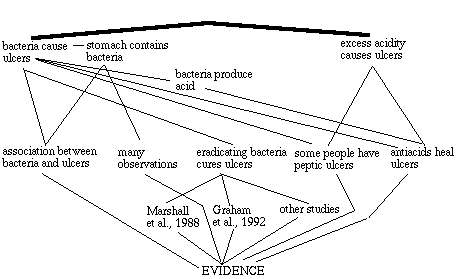
Figure 6. Coherence relations in assessing the acceptability of the hypothesis that bacteria cause ulcers in 1995. Thin lines indicated positive constraints based on hypotheses explaining evidence, and thick lines indicate negative constraints based on contradiction or competition.For a naturalistic explanation of belief change, the coherence account must be psychologically plausible. There is indirect evidence that it is, since parallel constraint satisfaction models using connectionist algorithms have been widely applied in recent work in cognitive science, to psychological phenomena that include word recognition, vision and imagery, analogy, language comprehension, and social impression formation (Holyoak and Spellman, 1993; Read and Marcus-Newhall, 1993; Schank and Ranney, 1992). Moreover, the explanatory coherence model ECHO has been used to account for the results of various psychological experiments. Hence, it is plausible that the belief change experienced by many medical researchers and practitioners concerning the cause of ulcers was produced by a process of assessing explanatory coherence.
I have shown how the hypothesis that Helicobacter pylori is the principal cause of peptic ulcers, which was largely rejected as absurd in 1983, could be on the way to medical orthodoxy in 1995. Satisfying Koch's postulates is not a necessary condition of showing that a microorganism causes a disease. Curing the disease by eliminating the microorganism is a powerful manipulation that provides substantial evidence that the microorganism causes the disease, and this kind of intervention has been repeatedly successful in the ulcers/bacteria case. However, accepting the hypothesis that bacteria cause ulcers is not just a matter of appreciating one kind of evidence, but rather of appreciating how the hypothesis coheres with various kinds of evidence and with other hypotheses. For most researchers, the claim that ulcers cause bacteria was not part of the most coherent account in 1983, but it is maximally coherent in 1996.
Cognitive coherence is, however, only part of the story about why the bacterial theory of ulcers has been increasingly accepted. This paper has treated belief change as a largely psychological phenomenon, a process in the minds of medical researchers. But the development of medical science also requires attention to the interactions of researchers with the world by means of instruments and experiments and the social interactions of researchers with each other and other parts of society (see Thagard, forthcoming-b). A full naturalistic account of the rise of the bacterial theory of ulcers should eventually specify how the cognitive aspects of belief formation and change described in this paper interact with the physical and social aspects of the development of science.
(1) Steer and Colin-Jones (1975) reported finding bacteria in gastric epithelium and observed their correlation with gastric ulceration, but misidentified them as Pseudomonas aeruginosa. Warren and Marshall's research, which led to the culturing, correct identification, and clinical assessment of the bacteria, was done independently of this previous work.
(2) Eliasmith and Thagard (in press) argue that the acceptance of the wave theory of light is much better understood in coherence terms than in probabilistic terms. This paper also includes the rigourous characterization of coherence as constraint satisfaction formulated in Thagard and Verbeurgt (forthcoming). I have run computer simulations to show that maximizing coherence given the relations in figure 2 leads to rejection of the hypothesis that bacteria cause ulcers, and that maximizing coherence given the relations in figure 3 leads to its acceptance.
BonJour, L. (1985). The structure of empirical knowledge. Cambridge, MA: Harvard University Press.
Brock, T. D. (Ed.). (1961). Milestones in microbiology. Englewood Cliffs, NJ: Prentice-Hall.
Brock, T. D. (1988). Robert Koch: A life in medicine and bacteriology. Madison, WI: Science Tech Publishers.
Bromberger, S. (1992). On what we know we don't know: Explanation, theory, linguistics, and how questions shape them. Chicago: University of Chicago Press.
Campbell, D. (1988). Methodology and epistemology for social science: Selected papers. Chicago: University of Chicago Press.
Coghlan, J. G., Gilligan, D., Humphries, H., McKenna, D., Dooley, C., Sweeney, E., Keane, C., & O'Morain, C. (1987). Campylobacter pylori and recurrence of duodenal ulcers: A 12 month follow-up study. Lancet (8568), 1109-1111.
Cover, T. L., & Blaser, M. J. (1992). Helicobacter pylori and gastroduodenal disease. Annual Review of Medicine, 43, 133-145.
de Boer, W., Driessen, W., Jansz, A., & Tytgat, G. (1995). Effect of acid suppression on efficacy of treatment for Helicobacter pylori infection. Lancet, 345, 817-820.
Eliasmith, C., & Thagard, P. (in press). Waves, particles, and explanatory coherence. British Journal for the Philosophy of Science.
Elwood, J. M. (1988). Causal relationships in medicine. Oxford: Oxford University Press.
EUROGAST Study Group (1993). An international association between Helicobacter pylori infection and gastric cancer. Lancet, 341(8857), 1359-1362.
Evans, A. S. (1993). Causation and disease: A chronological journey. New York: Plenum.
Forbes, G. M., Glaser, M. E., Cullen, D. J. E., Warren, J. R., Christianson, K. J., & Marshall, B. J. (1994). Duodenal ulcer treated with Helicobacter pylori eradication: Seven year follow-up. Lancet, 342, 258-260.
Forman, D. et al. (1991). Association between infection with Helicobacter pylori and risk of gastric cancer: Evidence from a prospective investigation. British Medical Journal, 302, 1302-1305.
Fung, W. P., Papadimitriou, J. M., & Matz, L. R. (1979). Endoscopic, histological, and ultrastructural correlations in chronic gastritis. American Journal of Gastroenterology, 71, 269-279.
Goodwin, C. S., Armstrong, J. A., Chilvers, T., Peters, M., Collins, M. D., Sly, L., McConnell, W., & Harper, W. E. S. (1989). Transfer of Campylobacter pylori and Campylobacter mustelae to Helicobacter gen. nov. as Helicobacter pylori comb. nov and Helicobacter mustelae comb. nov., Respectively. International Journal of Systematic Bacteriology, 39, 397-405.
Graham, D. Y. (1990). Present status of research and outlook for the future: What did we accomplish? In F. Halter, A. Garner, & G. N. J. Tytgat (Eds.), Mechanisms of peptic ulcer healing (pp. 303-309). Dordrecht: Kluwer.
Graham, D. Y. (1991). Helicobacter pylori: Its epidemiology and its role in duodenal ulcer disease. Journal of Gastroenterology and Hepatology, 6, 105-113.
Graham, D. Y. (1993). Treatment of peptic ulcers caused by Helicobacter pylori. New England Journal of Medicine, 328, 349-350.
Graham, D. Y. (1996). in press. Annual Review of Medicine.
Graham, D. Y., & Go, M. F. (1993). Helicobacter pylori: Current status. Gastroenterology, 105, 279-282.
Graham, D. Y., Lew, G. M., Klein, P. D., Evans, D. G., Evans, D. J., Saeed, Z. A., & Malaty, H. M. (1992). Effect of treatment of Helicobacter pylori infection on long-term recurrence of gastric or duodenal ulcer: A randomized, controlled study. Annals of Internal Medicine, 116, 705-708.
Graham, J. R. (1995). Helicobacter pylori: Human pathogen or simply an opportunist? Lancet, 345, 1095-1097.
Harman, G. (1986). Change in view: Principles of reasoning. Cambridge, MA: MIT Press/Bradford Books.
Hentschel, E., Brandstätter, G., Dragosics, B., Hirschl, A. M., Nemec, H., Schütze, K., Taufer, M., & Wurzer, H. (1993). Effect of ranitidine and amoxicillin plus metronidazole on the eradication of Helicobacter pylori and the recurrence of duodenal ulcer. New England Journal of Medicine, 328(308-312).
Hintikka, J., & Vandamme, F. (Ed.). (1985). Logic of discovery and logic of discourse. New York: Plenum.
Holland, J. H. (1975). Adaptation in natural and artificial systems. Ann Arbor: University of Michigan Press.
Holland, J. H., Holyoak, K. J., Nisbett, R. E., & Thagard, P. R. (1986). Induction: Processes of inference, learning, and discovery. Cambridge, MA: MIT Press/Bradford Books.
Holyoak, K. J., & Spellman, B. A. (1993). Thinking. Annual Review of Psychology, 44, 265-315.
Holyoak, K. J., & Thagard, P. (1995). Mental leaps: Analogy in creative thought. Cambridge, MA: MIT Press/Bradford Books.
Hosking, S. W., Ling, T. K. W., Chung, S. C., Cheng, A. F., & Sung, J. J. (1994). Duodenal ulcer healing by eradication of Helicobacter pylori without anti-acid treatment: Randomised controlled trial. Lancet, 343, 508-510.
Kahneman, D., Slovic, P., & Tversky, A. (1982). Judgment under uncertainty: Heuristics and biases. New York: Cambridge University Press.
Kantorovich, A. (1993). Scientific discovery: Logic and tinkering. Albany: State University of New York Press.
Klahr, D., & Dunbar, K. (1988). Dual space search during scientific reasoning. Cognitive Science, 12, 1-48.
Kleiner, S. A. (1993). The logic of discovery: A theory of the rationality of scientific research. Dordrecht: Kluwer.
Koza, J. R. (1992). Genetic programming. Cambridge, MA: MIT Press.
Kunda, Z., Miller, D., & Claire, T. (1990). Combining social concepts: The role of causal reasoning. Cognitive Science, 14, 551-577.
Langley, P., Simon, H., Bradshaw, G., & Zytkow, J. (1987). Scientific discovery. Cambridge, MA: MIT Press/Bradford Books.
Lauer, T. W., Peacock, E., & Graesser, A. C. (Ed.). (1992). Questions and information systems. Hillsdale, NJ: Erlbaum.
Lehrer, K. (1990). Theory of knowledge. Boulder: Westview.
Marshall, B. J. (1989). History of the discovery of C. pylori. In M. J. Blaser (Eds.), Campylobacter pylori in gastritis and peptic ulcer disease (pp. 7-22). New York: Igaku-Shoin.
Marshall, B. J. (1994). Helicobacter pylori. American Journal of Gastroenterology.
Marshall, B. J., Armstrong, J. A., McGechie, D. B., & Clancy, R. J. (1985). Attempt to fulfil Koch's postulates for pyloric campbylobacter. Medical Journal of Australia, 142, 436-439.
Marshall, B. J., Barrett, L. J., Prakash, C., McCallum, R. W., & Guerrant, R. L. (1990). Urea protects Helicobacter (Campylobacter) pylori from the bactericidal effect of acid. Gastroenterology, 99, 697-702.
Marshall, B. J., Goodwin, C. S., Warren, J. R., Murray, R., Blincow, E. D., Blackbourn, S. J., Phillips, M., Waters, T. E., & Sanderson, C. R. (1988). Prospective double-blind trial of duodenal ulcer relapse after eradication of campylobacter pylori. Lancet, 2(8626/8627), 1437-1441.
Marshall, B. J., & Warren, J. R. (1984). Unidentified curved bacilli in the stomach of patients with gastritis and peptic ulceration. Lancet, 1(8390), 1311-1315.
Monmaney, T. (1993, September 20). Marshall's hunch. New Yorker, p. 64-72.
National Institutes of Health Consensus Development Panel (1994). Helicobacter pylori in peptic ulcer disease. Journal of the American Medical Association, 272, 65-69.
Newell, A., & Simon, H. A. (1972). Human problem solving. Englewood Cliffs, NJ: Prentice-Hall.
Olbe, L., Hamlet, A., Dalenbäck, J., & Fändriks, L. (1996). A mechanism by which Helicobacter pylori infection of the antrum contributes to the development of duodenal ulcer. Gastroenterology, 110, 1386-1394.
Peterson, W. L. (1991). Helicobacter pylori and peptic ulcer disease. New England Journal of Medicine, 324, 1043-1048.
Ram, A. (1991). A theory of questions and question asking. Journal of the Learning Sciences, 1, 273-318.
Rauws, E. A. J., & Tytgat, G. N. J. (1990). Cure of duodenal ulcer with eradication of Helicobacter pylori. Lancet, 335(8700), 1233-1235.
Read, S., & Marcus-Newhall, A. (1993). The role of explanatory coherence in the construction of social explanations. Journal of Personality and Social Psychology, 65, 429-447.
Roberts, R. M. (1989). Serendipity: Accidental discoveries in science. New York: Wiley.
Salmon, W. (1984). Scientific explanation and the causal structure of the world. Princeton: Princeton University Press.
Schaffner, K. F. (1993). Discovery and explanation in biology and medicine. Chicago: University of Chicago Press.
Schank, P., & Ranney, M. (1992). Assessing explanatory coherence: A new method for integrating verbal data with models of on-line belief revision. In Proceedings of the Fourteenth Annual Conference of the Cognitive Science Society (pp. 599-604). Hillsdale, NJ: Erlbaum.
Schunn, C. D., & Klahr, D. (1995). A 4-space model of scientific discovery. In J. D. Moore & J. F. Lehman (Eds.), Proceedings of the Seventeenth Annual Conference of the Cognitive Science Society (pp. 106-111). Mahwah, NJ: Erlbaum.
Simon, H. A., & Lea, G. (1974). Problem solving and rule induction: A unified view. In L. W. Gregg (Eds.), Knowledge and cognition Hillsdale, NJ: Erlbaum.
Steer, H. W. & Colin-Jones, D. G. (1975). Mucosal changes in gastric ulceration and their response to carbenoxolone sodium. Gut, 16, 590-597.
Susser, M. (1973). Causal thinking in the health sciences. New York: Oxford University Press.
Suzuki, D. (1995). Ulcer wars (transcript of broadcast on CBC television). The Nature of Things (originally produced by BBC TV).
Thagard, P. (1988). Computational philosophy of science. Cambridge, MA: MIT Press/Bradford Books.
Thagard, P. (1989). Explanatory coherence. Behavioral and Brain Sciences, 12 , 435-467.
Thagard, P. (1992). Conceptual revolutions. Princeton: Princeton University Press.
Thagard, P. (forthcoming-a). The concept of disease: Structure and change. Communication and Cognition.
Thagard, P. (forthcoming-b). Ulcers and bacteria II: Instruments, experiments, and social interactions. Studies in History and Philosophy of Science.
Thagard, P., & Verbeurgt, K. (forthcoming). Coherence. Under review.
Warren, J. R., & Marshall, B. J. (1983). Unidentified curved bacilli on gastric epithelium in active chronic gastritis. Lancet, 1 (8336), 1273-1275.